A lot of adults were never taught accurate anatomy. Many people grow up hearing vague words, slang, or incomplete explanations—then feel embarrassed to ask questions later. But anatomy knowledge isn’t “awkward trivia.” It’s basic health literacy. It helps you communicate clearly with partners and healthcare providers, recognize what’s normal for you, spot problems early, and make safer choices.
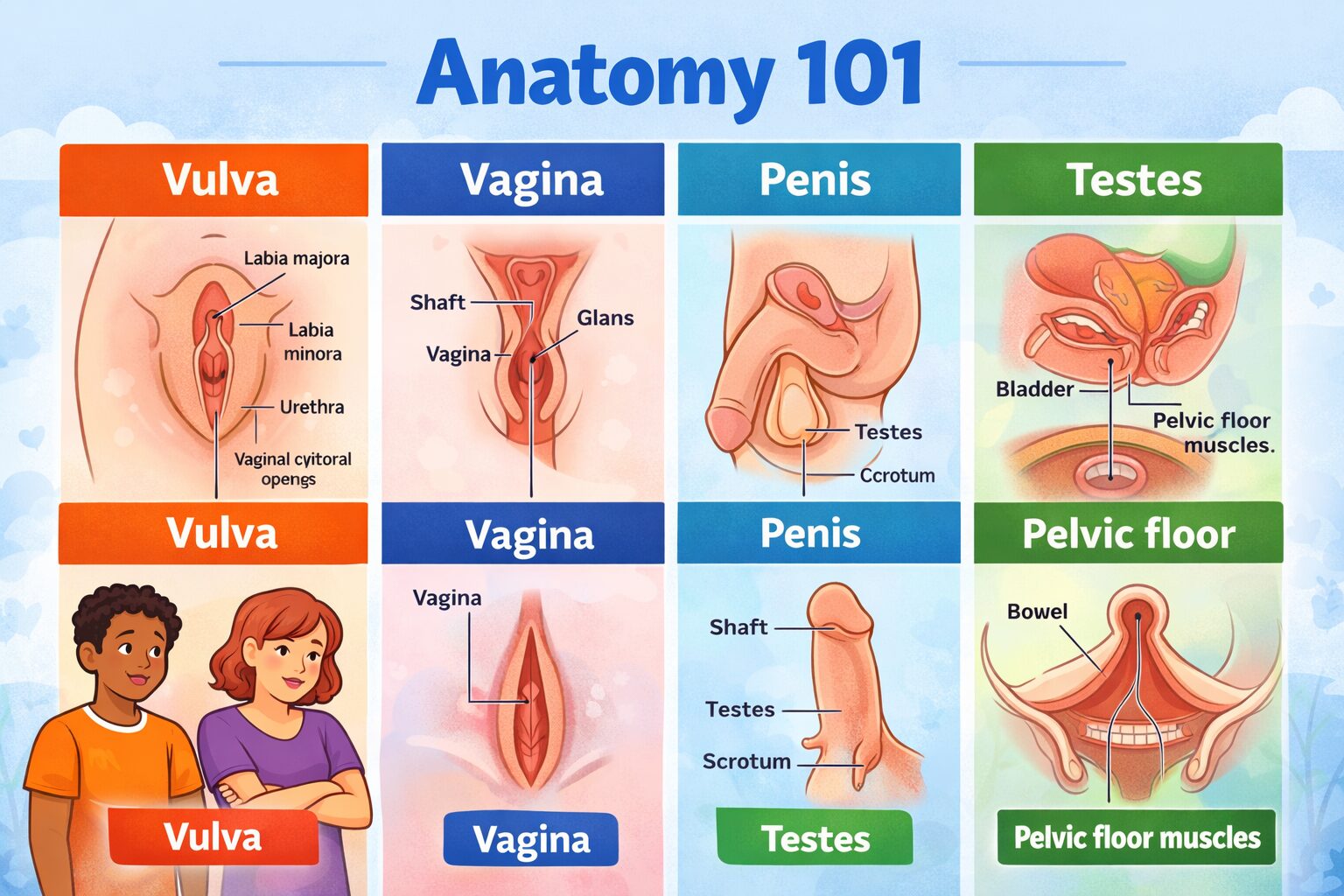
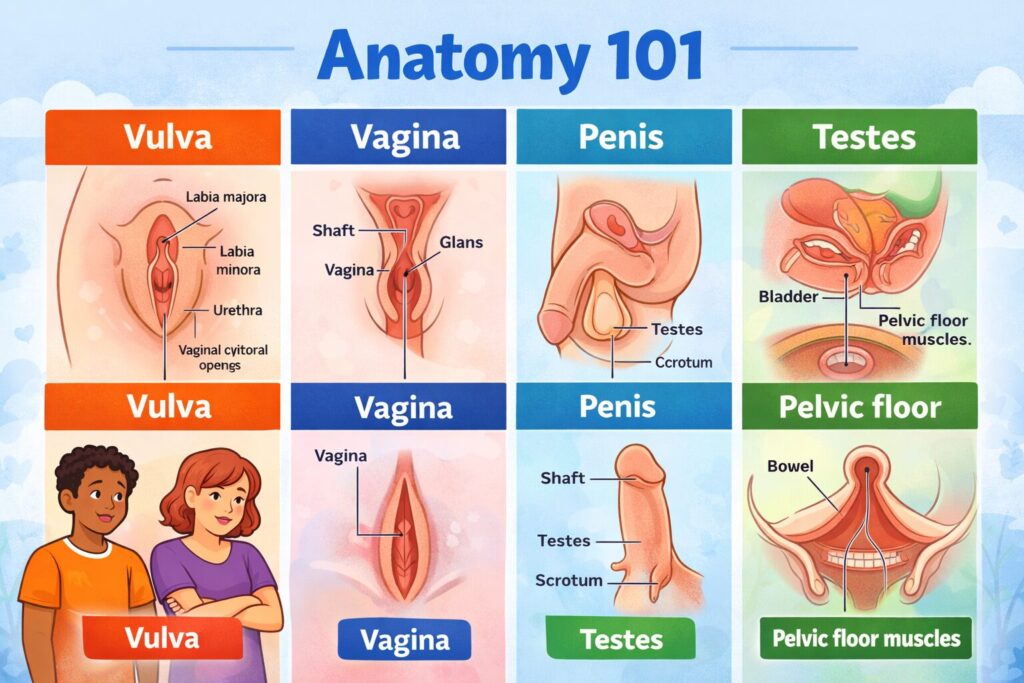
This Anatomy 101 guide explains the vulva and vagina, penis and testes, the clitoris, and the pelvic floor using clear, inclusive, non-graphic language. If you’ve ever mixed up terms (you’re not alone), this will make it simple.
Quick Answer (Featured Snippet)
Anatomy 101 explains the difference between external genital anatomy (like the vulva or penis) and internal anatomy (like the vagina), plus key structures like the clitoris and the pelvic floor. The vulva is external; the vagina is internal. Testes produce sperm and hormones; the penis is external. The clitoris is a sensitive organ with internal parts. The pelvic floor supports bladder, bowel, and sexual function.
Key Takeaways
- The vulva is external anatomy; the vagina is an internal canal.
- The clitoris is larger than most people realize, with internal structures.
- Penis and testes have different roles: urination, sexual function, hormones.
- The pelvic floor is a muscle group supporting bladder, bowel, and pelvic organs.
- Accurate terms improve healthcare, communication, safety, and confidence.
Table of Contents
- What “Anatomy 101” Means (Plain Explanation)
- Why It Matters (Real-Life Impact)
- The Basics You Need to Know (Simple Definitions)
- Vulva vs Vagina (Clear Differences)
- Penis vs Testes (Clear Differences)
- The Clitoris (What It Is and Why It Matters)
- The Pelvic Floor (Support System and Function)
- Step-by-Step: How to Learn Your Anatomy Safely
- Common Myths and Mistakes
- Safety, Consent, and Boundaries
- When to See a Doctor or Professional Help
- FAQ
- Final Take + Next Step
1) What “Anatomy 101” Means (Plain Explanation)
“Anatomy 101” means learning the basic structures of the body using correct names and clear definitions. In this article, we focus on:
- Vulva and vagina (often confused)
- Penis and testes (different roles)
- Clitoris (often misunderstood)
- Pelvic floor (muscles that support key functions)
This is educational and non-graphic. It’s about health, communication, and understanding your body.
Inclusive note: People’s bodies vary widely. Not everyone fits typical categories, and intersex variations exist. Anatomy knowledge helps everyone, regardless of identity.
2) Why It Matters (Real-Life Impact)
Knowing anatomy helps you:
- describe symptoms clearly to a clinician
- reduce shame and confusion (“What’s normal?”)
- understand how arousal, comfort, and pain can work
- identify red flags early (infection, lumps, unusual pain)
- communicate boundaries and preferences respectfully
- feel more confident in healthcare and relationships
It also protects safety: when people can name body parts, it becomes easier to explain boundaries and report harm.
[Internal link: What Is Sex Education (and What It Is Not)]
[Internal link: Sexual Consent Basics—Clear, Practical Guide]
3) The Basics You Need to Know (Simple Definitions)
Here are quick, clear definitions you can come back to:
- Vulva: external genital anatomy (outside).
- Vagina: internal canal leading to the cervix (inside).
- Penis: external organ involved in urination and sexual function.
- Testes (testicles): glands that produce sperm and testosterone (usually in the scrotum).
- Clitoris: a sensitive organ with external and internal parts.
- Pelvic floor: a group of muscles that support pelvic organs and control openings.
Key concept: external and internal parts are different structures. Using the right term avoids confusion.
4) Vulva vs Vagina (Clear Differences)
Many people use “vagina” to mean everything in that area, but medically:
- Vulva = outside
- Vagina = inside
The vulva (external anatomy)
The vulva includes:
- Labia majora (outer folds of skin)
- Labia minora (inner folds; size and shape vary a lot)
- Clitoral glans (the visible tip of the clitoris)
- Urethral opening (where urine exits)
- Vaginal opening (entrance to the vagina)
- Perineum (area between vaginal opening and anus)
Normal variation: Labia come in many shapes, sizes, and colors. Asymmetry is common. “Normal” is a wide range.
The vagina (internal anatomy)
The vagina is a muscular canal that:
- connects the vulva to the cervix
- allows menstrual flow to leave the body
- can stretch (for example, during childbirth)
- changes with hormones across life stages
A common misconception is that the vagina is “loose” or “tight” based on sexual history. In reality, vaginal comfort is influenced by many factors—stress, arousal, hormones, pelvic floor muscles, and medical conditions—not “body count.”
5) Penis vs Testes (Clear Differences)
The penis (external anatomy)
The penis is an external organ that can be involved in:
- urination (via the urethra)
- sexual function (including erections and sensation)
The penis includes:
- Shaft (main length)
- Glans (tip)
- Foreskin (in some people; can be circumcised or not)
- Urethral opening (where urine and semen exit)
Normal variation: Size, shape, curve, and appearance vary widely. Many curves are normal.
The testes (testicles)
Testes are glands usually located in the scrotum. Their main roles:
- produce sperm
- produce testosterone and other hormones
It’s normal for one testis to hang lower than the other. It can also be normal to notice temperature-related changes in how the scrotum sits.
6) The Clitoris (What It Is and Why It Matters)
The clitoris is one of the most misunderstood body parts. Many people think it’s only a small external “button,” but it’s actually a larger structure with internal components.
What the clitoris is
The clitoris is a sensitive organ involved in sexual pleasure for many people. It includes:
- External part: the clitoral glans (the visible portion)
- Internal parts: structures that extend inside the body (often described as “legs” and bulbs)
You don’t need to memorize every term to understand the key point:
Most of the clitoris is internal.
Why this matters for health education
Understanding clitoral anatomy helps people:
- recognize that comfort and sensation vary
- communicate better about what feels okay (and what doesn’t)
- reduce myths that pressure people into one “normal” experience
No one owes any specific response. Bodies vary.
7) The Pelvic Floor (Support System and Function)
The pelvic floor is a group of muscles like a supportive hammock at the base of the pelvis. It supports:
- bladder
- bowel
- uterus (if present)
- sexual function and sensation
- core stability and posture
Signs your pelvic floor may need attention
Pelvic floor issues can affect anyone (people with vulvas or penises). Signs can include:
- urinary leakage (especially when coughing/laughing/exercising)
- pelvic heaviness or pressure
- pain in the pelvis or during intercourse
- difficulty fully emptying bladder or bowel
- ongoing constipation or straining
- erectile difficulties linked to tension, pain, or circulation issues
These symptoms are common—and treatable. Pelvic floor physical therapy can be a game-changer for many people.
8) Step-by-Step: How to Learn Your Anatomy Safely
This is about comfort, health, and clarity—not perfection.
Step 1: Use correct terms in low-pressure moments
Start by practicing language privately:
- “vulva” for outside
- “vagina” for inside
- “testes” for the glands
- “pelvic floor” for the muscle group
Step 2: Learn what’s normal for your body
Noticing your baseline helps you spot changes:
- skin changes
- new lumps
- unusual pain
- changes in discharge (for people with vaginas)
- persistent itching or burning
- swelling that doesn’t go away
Step 3: If something changes, write it down
Symptoms to note:
- when it started
- what makes it better/worse
- any fever, pain, or discharge
- whether it affects urination or bowel movements
Clear notes help clinicians help you faster.
Step 4: Ask a clinician directly when needed
If you don’t know which term to use, describe location:
- “outside near the opening”
- “internal discomfort”
- “testicular ache”
- “pelvic pressure”
Clinicians hear this every day. You’re not “weird” for asking.
Checklist: Anatomy confidence essentials
- ☐ I know vulva vs vagina difference
- ☐ I know penis vs testes difference
- ☐ I know the clitoris has internal parts
- ☐ I know what pelvic floor means
- ☐ I can describe symptoms clearly
- ☐ I know when to seek professional help
9) Common Myths and Mistakes
Myth vs Fact (Decision Table)
| Myth | Fact | Better next step |
|---|---|---|
| “Vagina means everything outside too.” | Vulva is external; vagina is internal. | Use the correct term for clarity. |
| “Clitoris is just a tiny external spot.” | Most clitoral tissue is internal. | Learn the basic structure; no need for shame. |
| “Labia should look a certain way.” | Labia vary widely; asymmetry is common. | Avoid comparison; focus on health and comfort. |
| “Testicular pain is always normal.” | Persistent pain deserves evaluation. | Seek medical advice if it lasts or worsens. |
| “Pelvic floor problems only happen after childbirth.” | They can affect anyone at any age. | Consider pelvic floor assessment if symptoms appear. |
Common mistakes
- Using vague language with clinicians
Better: describe location and symptoms precisely. - Ignoring persistent itching, pain, or swelling
Better: treat ongoing symptoms as a reason to get checked. - Assuming porn teaches anatomy
Better: use health education sources and clinicians. - Feeling embarrassed to ask
Better: practice terms; it gets easier quickly.
10) Safety, Consent, and Boundaries
Anatomy education supports consent because it helps people:
- name body parts and boundaries clearly
- recognize discomfort and speak up
- understand that “stop” is always valid
- seek help if something feels wrong
Consent and boundaries apply to:
- physical touch
- sexual activity
- medical exams (you can ask questions and request pauses)
- digital sharing (photos, messages)
[Internal link: Consent and Boundaries—Practical Scripts]
[Internal link: Online Safety and Digital Consent Basics]
11) When to See a Doctor or Professional Help
Most anatomy variation is normal. But some symptoms shouldn’t be ignored.
Red flags (seek care promptly)
- new lump in a testis or scrotum
- severe or worsening pelvic or genital pain
- fever plus pelvic/genital symptoms
- persistent burning with urination
- unusual bleeding
- sores, blisters, or rash that doesn’t improve
- swelling, redness, or warmth that spreads
- ongoing pain during intercourse
- urinary leakage that interferes with life
Brief safety note: If you feel unsafe, coerced, or at risk of harm, prioritize immediate safety and contact local emergency services or a trusted support professional.
12) FAQ
1) Is it normal to confuse vulva and vagina?
Yes. Many people were taught incorrect or vague terms. The vulva is external anatomy; the vagina is the internal canal. Using accurate words helps with healthcare, boundaries, and confidence. It’s never “too late” to learn the correct terms.
2) Is it normal for labia to look uneven?
Yes. Labia size, color, and symmetry vary widely. Asymmetry is common and usually not a health issue. If you notice sudden swelling, pain, new lumps, or persistent irritation, that’s when a clinician can help you rule out infection or skin conditions.
3) What should I do if I notice a testicular lump?
Get it checked promptly by a healthcare professional. Many lumps are not cancer, but it’s important not to guess. Note whether it’s painful, hard, or changing size, and whether you have fever or swelling. Early evaluation is the safest approach.
4) Can the clitoris be “too sensitive”?
Sensitivity varies. Temporary sensitivity can change with hormones, stress, friction, infections, or skin irritation. If sensitivity becomes painful, persistent, or disruptive, a clinician can help check for irritation, infection, or nerve-related issues and suggest supportive care.
5) Can pelvic floor problems affect people with a penis?
Yes. Pelvic floor muscles affect bladder control, bowel function, and sexual function for everyone. Tension, weakness, or coordination problems can contribute to pain, urinary symptoms, or erectile issues. Pelvic floor physical therapy can be helpful and is worth discussing with a clinician.
6) Is pain during intercourse always normal?
No. Discomfort can happen sometimes, but ongoing pain should be evaluated. Causes can include dryness, pelvic floor tension, infections, inflammation, hormonal changes, or other conditions. A clinician can help you identify the cause and treatment options safely.
7) Does penis size affect fertility or function?
Not necessarily. Fertility is more related to sperm health, hormones, and overall reproductive function than penis size. Sexual function depends on many factors like circulation, nerves, stress, and communication. If you’re concerned about function, a clinician can offer evidence-based guidance.
8) When should I see a pelvic floor specialist?
Consider it if you have leakage, pelvic pressure, persistent constipation/straining, pain, or discomfort during intercourse. Pelvic floor physical therapists assess muscle strength, tension, and coordination and can teach exercises and strategies tailored to your body and symptoms.
13) Final Take + Next Step
Accurate anatomy knowledge is a form of self-respect. It helps you communicate clearly, recognize issues early, and make safer, healthier choices. The big takeaways are simple:
- vulva is external, vagina is internal
- penis and testes have different roles
- the clitoris includes internal structures
- the pelvic floor supports bladder, bowel, and sexual function
Next step: Pick one term you’ve avoided (like “vulva” or “pelvic floor”) and practice using it calmly. If you have a persistent symptom you’ve been ignoring, make a plan to get it checked.